Newborn jaundice (yellowing of the skin and whites of the eyes) is quite common in newborn babies as all babies are born with more red blood cells than they need for life outside the uterus, and these are broken down releasing the yellow pigment bilirubin. If levels of bilirubin climb too high however it could be dangerous for your baby. Getting breastfeeding established promptly can help reduce the risk of high levels of bilirubin, see A Good Start to Breastfeeding and Breastfeeding Tips for Newborns for help to get breastfeeding off to a good start or contact your IBCLC lactation consultant for one-to-one help.
This article discusses the options for treatment for jaundice when it is needed. For further reading about symptoms of jaundice and what causes it see Causes and Symptoms of Jaundice. For a summary of how breastfeeding can affect jaundice see Jaundice in Breastfeeding Babies.
When does jaundice require treatment?
Bilirubin levels can be measured and serve as a guide to treatment when they cross a certain threshold. The baby’s medical team will also take account of each baby’s medical situation. The baby’s age, whether premature, their weight, when the jaundice started, and whether the baby is feeding well along with any maternal and infant health factors will all be considered before deciding when to start treatment.1
If breastfeeding is going well, and the bilirubin levels are dropping naturally, treatment may not be needed. A paper from Lawrence Gartner, 2001 explains:
In the full-term healthy infant, phototherapy and complementary or substitution feedings with infant formula are not needed until serum levels exceed 300 to 340 µM/L (18 to 20 mg/dL). Even when slightly greater than 340 µM/L ( 20 mg/dL), but not rising rapidly, further observation and assurance of good breastmilk intake may be all that is required. Hemolysis and other pathologic causes of hyperbilirubinemia must be ruled out, of course.
Lower levels may be of concern in premature babies and/or babies with other health issues. 2 If the need for treatment for jaundice is identified, this may involve phototherapy, supplementation with milk or exchange transfusion (blood transfusion).
Official guidance on thresholds for treatment
Documents with treatment guidelines that are supportive of preserving breastfeeding include:
NICE Guidelines
National Institute for Health and Care Excellence (NICE) recommendations can be found in Jaundice in Newborn Babies Under 28 Days (2023) and Neonatal Jaundice Clinical Guidance (2010).
Their information includes a threshold table and treatment threshold graphs to assess and treat jaundice based on bilirubin levels found in the blood.
Academy of Breastfeeding Medicine guidelines
The Academy of Breastfeeding Medicine (ABM) 2017 also has guidelines for managing jaundice over 35 weeks gestation.
How is bilirubin measured?
Visually checking for jaundice—by noting the progression of yellow pigment from head towards the lower body—is not as accurate as measuring the levels in the following ways:
- Total serum bilirubin (TSB) is the amount of bilirubin in the blood and is measured by a blood test. Blood is usually collected by a heel prick sometimes called an “SB” or a “bili” test. A split bilirubin test shows whether the cause of the jaundice is liver disease by measuring the ratios of the conjugated and unconjugated bilirubin levels in your baby’s blood.
- Transcutaneous bilirubin (TcB) is the level of yellow bilirubin in the skin measured with a transcutaneous bilirubinometer
NICE guidelines advise which of these tests to use in which circumstances and caution against using umbilical cord blood bilirubin level, end-tidal carbon monoxide (ETCOc) measurement or umbilical cord blood direct antiglobulin test (DAT) (Coombs’ test) as ways to predict significant jaundice.
Treatment for Jaundice
#1 Phototherapy
Phototherapy is a treatment that uses blue spectrum light to lower bilirubin levels. The baby’s skin absorbs the light waves which break down bilirubin molecules in the body into a water soluble form that the body can get rid of more easily via the bowel (in poop!).
Phototherapy normally works well to drop the bilirubin levels quickly and a couple of days of treatment may be all that are needed. Although a baby may tend to lose more fluids while under the lights, babies don’t routinely need any extra fluids by mouth or intravenously during therapy (ABM, 2017). Breastfeeding can continue. Short breaks for breastfeeding, changing nappies and contact with parents will be encouraged (NICE, 2023).
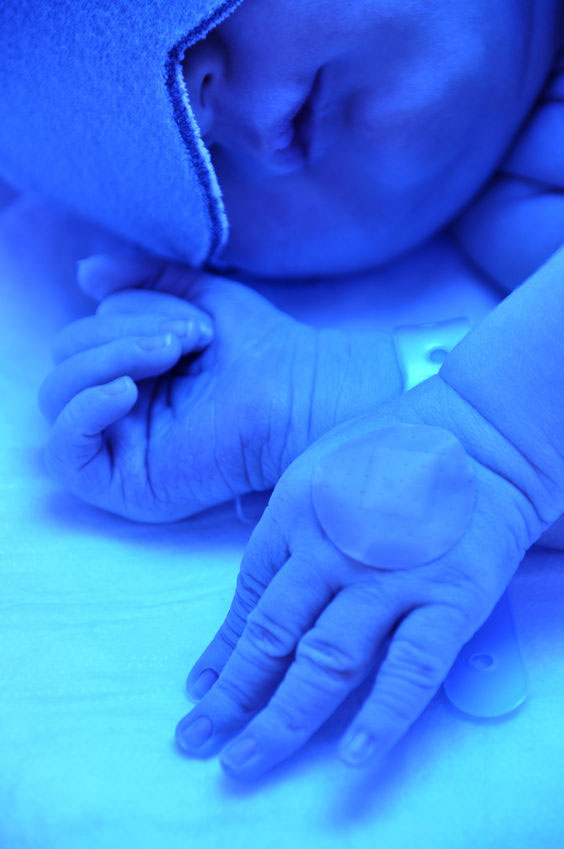
Is phototherapy safe?
Phototherapy is reported to be very effective with few side effects. Babies will be carefully monitored for overheating, or dehydration by the health care team.3
Green poop
Linda Palmer points out that there may be plenty of green poop when bilirubin is excreted.4
A note on sunlight
NICE Guidelines do not advise using sunlight as a treatment for jaundice, and the American Academy of Paediatrics say:
Putting your baby into sunlight is not a safe way to treat jaundice.
#2 Supplementation (extra milk)
If one of the causes of a baby’s jaundice is not enough milk intake (starvation jaundice), a baby may need to be supplemented with pumped breast milk, donor breast milk or cows’ milk formula in addition to the mother working with an IBCLC lactation consultant to increase her milk supply. Jaundice can also make a baby sleepy which can prevent them from feeding well5 and a mother may need to pump her milk in these circumstances to maintain or increase her supply to provide sufficient milk for her baby.
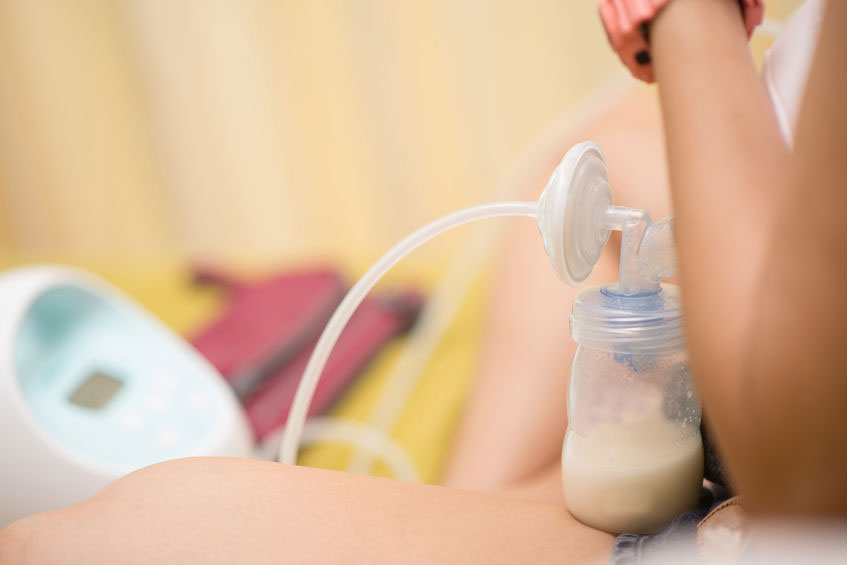
Flaherman and Kair explain that whatever the cause of the jaundice, having plenty of calories will help. Therefore if breastfeeding is not going well any problems need to be addressed:
For neonates with jaundice attributable to poor breastmilk intake, the solution is not to stop the breastfeeding, but rather to correct the breastfeeding problem and to restore fluid and calorie intake. In some instances, expressed milk, banked donor human milk, or artificial milk (formula) supplementation may be required for a time.
Formula supplements?
The following protocol from the Academy of Breastfeeding Medicine explains why supplementing with formula may be suggested as an alternative to phototherapy to lower bilirubin levels in certain cases:
As infant formula inhibits the intestinal re- absorption of bilirubin, it may sometimes be used to lower TSB in breastfeeding infants. Small-volume (10–15 mL) feedings of formula immediately following a breastfeeding may be preferred to intermittent large-volume (30–60 mL) supplementation so as to maintain frequent breastfeeding and preserve maternal milk production at a high level. Larger volumes may be required if the infant is not receiving sufficient milk…
The ABM protocol states that the first and best supplement is mother’s expressed breast milk to avoid undermining breastfeeding. Donor milk is the next favoured option if more breast milk is needed. The supplements can be fed by cup (baby must be alert and awake), syringe, supplemental nursing system, finger feed, or bottle to ensure the baby is getting plenty of calories.

Cautions re water
The AAP says supplementing a baby with water or glucose (dextrose) water will not prevent jaundice or lower the bilirubin levels because bilirubin is excreted in poop and not urine and the harms will exceed the benefits.6 If a mother’s milk is delayed coming in or if she doesn’t have enough milk she may need to supplement with donor milk or infant formula alongside any treatments needed.
#3 Blood transfusions
Exchange transfusions (blood transfusions) are rarely performed today as phototherapy is so effective. Guidelines and risks for exchange transfusion are clarified in:
Is stopping breastfeeding for a while ever necessary?
Breastfeeding can usually continue alongside other treatments and temporary weaning should rarely be necessary.78
The NICE guidelines say continue breastfeeding during phototherapy, give the mother good breastfeeding support and that mothers’ expressed breast milk should be the first choice if additional feeds are indicated. 9
Interrupting breastfeeding?
Occasionally a baby’s health professionals may advise interrupting breastfeeding for a short period (24 to 48 hours) in specific situations. The Academy of Breastfeeding Medicine jaundice protocol states:
Temporary interruption of breastfeeding is very rarely needed, but may be considered for specific clinical scenarios in which rapid reduction in TSB is urgently needed or if phototherapy is unavailable.
Pump to maintain supply
In the event of a pause in breastfeeding, pumping frequently will maintain a good supply of breast milk ready for when breastfeeding resumes.
Summary
It’s quite normal for newborn babies to have a little jaundice as they are born with extra blood cells that are no longer needed after birth. The breakdown of these blood cells in the baby’s liver releases a yellow pigment called bilirubin. The pigment is excreted in a baby’s poop and if breastfeeding is going well is not normally a problem. If levels of the pigment do get too high in certain circumstances, treatment will be needed to avoid complications.10 Treatment of newborn jaundice that is not associated with an underlying health problem usually involves phototherapy and/or supplementation. In most cases breastfeeding can and should continue alongside any treatment.