Small volumes of colostrum (the first breast milk) are usually enough for most newborn babies until their mothers’ milk arrives in larger volume on the second or third day of life. Sometimes however, there are situations where a baby may need additional milk feeds before his mother’s milk comes in. For example a baby born to a diabetic mother might be born with low blood sugar, and need food quickly to address this. Expressing and storing colostrum antenatally (before birth) means the perfect food will be available if needed, and avoids having to use infant formula. Avoiding formula where possible is desirable as it is an industrially made substance missing the important protective factors, hormones and friendly bacteria that a newborn baby needs at birth.
This article
This article looks at whether expressing colostrum during late pregnancy is safe, what the potential benefits could be and answers frequently asked questions.
What is colostrum? Colostrum is the first breast milk produced in the breast after a baby’s birth. Some mothers may notice they leak small amounts of colostrum many weeks or months before their baby is due.1 Colostrum is very good for a newborn baby, it is low in volume but each drop is rich in antibodies and concentrated nutrition. Colostrum helps the immune system develop and introduces friendly bacteria to colonise the gut to protect baby, it raises a baby’s blood sugars2 and acts as a laxative which helps to pass meconium (the first sticky black poop)3. Two or three days after the birth, the amount of colostrum in the breast increases and becomes mature breast milk over the next two weeks.4
What is antenatal expression of colostrum?
Antenatal expression involves hand expressing and collecting drops of colostrum from the breasts during late pregnancy. It is sometimes called harvesting colostrum or antenatal banking of colostrum.
Is antenatal expression safe?
Several National Health Service (NHS) foundation trusts in the UK advocate antenatal expression (see below), and several breastfeeding charities offer information on the subject.56 However, in breastfeeding literature, there are mixed opinions about the safety of harvesting colostrum in pregnancy. The main safety issue is that nipple stimulation releases oxytocin, a hormone that causes the uterus to contract in labour. There is a concern therefore that antenatal expression could potentially trigger premature labour resulting in complications from an early birth. Those who advocate antenatal expression usually recommend doing so in short sessions after about 36–37 weeks gestation—as long as there are no risk factors present for premature birth, and as long as the mother’s health care professional has no concerns.
Studies in favour
Singh et al, 2009 found antenatal expression once a day after 37 weeks gestation had positive benefits for breastfeeding 7 and a 2019 study in diabetic women found that learning to express in the last month of pregnancy can result in less formula use after birth.8 A study in 2017, known as the DAME study (Diabetes and Antenatal Milk Expressing), looked at the safety of antenatal expression amongst over 600 women with diabetes in pregnancy and found:
There is no harm in advising women with diabetes in pregnancy at low risk of complications to express breastmilk from 36 weeks gestation.
Safety concerns
Previous to the studies above some authors and researchers expressed concerns about the safety of expressing colostrum in pregnancy. Lawrence and Lawrence9 say antenatal expression is a controversial procedure which could cause premature labour and occasionally antenatal mastitis, and the risks outweigh the benefits. Soltani and Scott10 found a higher rate of admission of babies to the special care baby unit (SCBU) when mothers expressed antenatally. And several other studies concluded that more research was needed before deciding whether antenatal expression was safe. 111213
Nipple stimulation and labour. Nipple stimulation, around the time a baby is due, can help induce labour and may also help ripen the cervix, reduce cesareans and reduce postpartum haemorrhage. There have been case studies where nipple stimulation has caused uterine hyperstimulation which could be harmful to the foetus, so the technique is not recommended for high-risk women.1415 Singh et al explain why oxytocin release from antenatal expression would be unlikely to cause labour contractions in the early antenatal period—because there are considerably fewer sites for oxytocin to be absorbed by the uterus (oxytocin receptors) before a mother’s due date. This may also be why intravenous oxytocin used to induce labour will not always work if the uterus isn’t ready. Another hormone, progesterone, also has a tight control on when birth will start, and the amount of nipple stimulation needed to trigger labour is thought to be much higher than that involved in antenatal expression (Singh, 2009).
Recent opinion
A recent review of the evidence in 2023 16 concluded that existing studies on antenatal expression are very limited and focus on women with diabetes rather than the general population. They conclude that although antenatal expression may be a useful tool to help breastfeeding succeed, there are also a number of disadvantages such as difficulty learning the technique, feeling defeated at small volumes expressed, discomfort or fear of pain, and feeling awkward while expressing. The paper concludes that more research is needed.
What about nipple stimulation via breastfeeding through pregnancy?
Nipple stimulation (and release of oxytocin) due to a mother continuing to breastfeed an older sibling during late pregnancy is not thought to trigger premature labour in a normal, low risk pregnancy 171819 The nipple stimulation from a breastfeeding toddler is likely to be at a higher frequency than occasional antenatal expression. For more reading see Can You Get Pregnant While Breastfeeding? on this website.
When considering antenatal expression for collection of colostrum it is important to do so in short sessions only (see below) and be guided by your health professionals for your individual situation.
What are the benefits of antenatal expression?
Collecting colostrum before birth can:
- Provide a breast milk supplement for after birth. Stored colostrum provides the perfect complete food a baby needs if for any reason he has difficulty breastfeeding or needs a supplement before his mother’s milk has “come in”.
- Prevent the need for industrially made formula and its associated disadvantages including changing the baby’s gut microbiome or increasing the risk of a baby developing allergies or diabetes.20
- Increase a mother’s confidence in hand expressing.21 Even if the drops of colostrum are not saved, once the technique of hand expression is learned, a mother can start hand expressing straight after the birth if her baby isn’t able to latch immediately.
- May help establish a full milk supply more quickly and get breastfeeding off to a good start (Singh, 2009)
Diabetes and antenatal expression
Antenatal expression of colostrum is often suggested for mothers with diabetes or gestational diabetes and research has focussed on this population. This is because some babies born to diabetic mothers can have low blood sugar levels22 and they benefit from a ready supply of colostrum as soon as possible. If baby’s blood sugar levels drop too low this is known as neonatal hypoglycaemia and can be dangerous for your baby. Breastfeeding as much as possible after birth is a good way to raise baby’s blood sugar levels and prevent hypoglycaemia. Because some diabetic mothers find their milk comes in later than usual23 and others find their baby isn’t ready to breastfeed yet, harvesting colostrum antenatally can ensure a supplement is available as needed. There are benefits for the mother too. Breastfeeding can help protect a mother with gestational diabetes from developing diabetes in later life and reduce the insulin a diabetic mother needs.24
In what situations might expressing colostrum be useful?
In addition to babies born to diabetic mothers, there could be other situations where having a little store of colostrum could be useful. A leaflet from Royal Berkshire NHS Foundation Trust suggests expressing colostrum if you:
- Have diabetes.
- Are receiving additional care or ultrasound scans due to the growth of their baby, large or small.
- Are taking Beta-blocker medication e.g. Labetalol.
- Have a planned Caesarean birth or an induced birth.
- Are expecting twins or multiples.
- Are anticipated to need Special Care admission.
- Are expected to have cleft lip or palate.
- Have a family history of metabolic disorders e.g. MCADD.
- Have any other medical conditions where challenges are anticipated (please discuss with your healthcare professional).
However, you should avoid expressing if you are at risk of pre-term labour.
When can I express colostrum?
It is usually recommended to start harvesting colostrum from around 36 to 37 weeks gestation. Mothers are advised to discuss their start date with their health care professionals in case they have any risk factors that mean antenatal expression should be avoided. For example if you have cervical incompetence or a cervical stitch in place, are expecting more than one baby (multiple pregnancy) or have a history of threatened or actual premature labour then antenatal expression is not recommended.2526
If a mother notices cramping pains during expressing, she should stop expressing and rest and discuss this with her health care professional.27
How do I express colostrum?
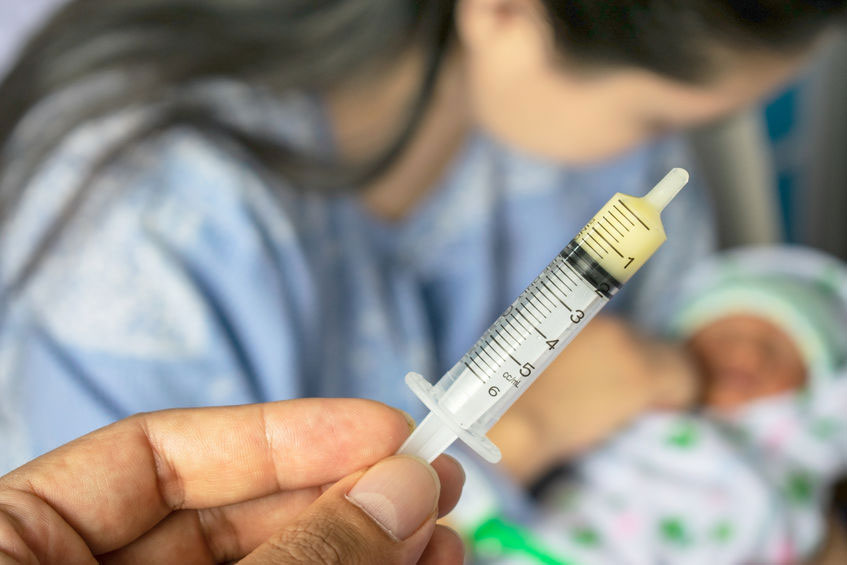
Hand expressing rather than pumping is the best way to collect colostrum as there will only be drops to collect at first and colostrum is thicker and stickier than mature breast milk. Labour is also more likely to be induced with high frequency pumping than gentle hand expression (Singh, 2009) and pumping is not recommended. The drops of expressed colostrum can be collected with a blunt ended sterile syringe or expressed onto a spoon or into a small cup and then drawn into a syringe for storage (Cox, 2006).
- For information and videos on techniques for hand expressing colostrum see Hand Expressing Breast Milk
- For an illustrated step by step guide to collecting and saving colostrum see Colostrum Harvesting (gestationaldiabetes.co.uk): scroll down to “How to Harvest Colostrum—Antenatal Expressing of Colostrum”.
How often can I express colostrum?
Information varies considerably from once a day (Cox, 2006) to at least four times a day (Wrightington, Wigan and Leigh NHS, 2019). Mothers in the DAME study expressed twice per day. La Leche League GB suggests expressing for three to five minutes up to three times a day (LLLGB, 2022). Your own NHS trust may have their own recommendations.
Some women find they can’t express colostrum before birth, this doesn’t mean they will have difficulty with breast milk production after birth.
How do I store colostrum?
Small sterile syringes can be used to collect colostrum to be frozen with the colostrum inside and thawed later as needed. After the birth, the syringe can be used to drip the colostrum into baby’s mouth. Maternity hospitals may be able to provide sterile syringes, or medical suppliers online provide individually wrapped small sterile syringes with or without caps.
For general storage information for breast milk see How Long Does Breast Milk Last? or ask your health professional.
Summary
Expressing colostrum before birth is known as antenatal expression. It involves expressing and storing drops of colostrum during late pregnancy. Having some stored colostrum after birth is a particular advantage to any baby likely to be born needing mothers’ milk quickly, for example babies born to diabetic mothers because they might have low blood sugar. Because nipple and breast stimulation in pregnancy could potentially start labour, historically there has been mixed advice about the safety and advisability of antenatal expression for fear of premature birth. Despite this, many National Health foundation trusts and breastfeeding charities have promoted this practice for low risk mothers for many years. Most organisations suggest antenatal expression be started after 36 to 37 weeks gestation. Harvesting colostrum is not recommended for high risk pregnancies, and there are a number of cautions to be aware of.
This article offers general information regarding antenatal expression of colostrum but it should not be construed as medical advice. Always discuss whether antenatal expression is appropriate for you with your own medical professionals who can advise you based on your medical history.