Jaundice (also called hyperbilirubinaemia) is the name given for the yellowing of the skin and whites of the eyes due to an accumulation of the brownish yellow pigment bilirubin. Newborn jaundice is common and is usually harmless.1 This article summarises the causes and symptoms of jaundice and is a companion article to Jaundice in Breastfeeding Babies and Treatment for Jaundice.
Causes of jaundice in newborn babies
During pregnancy the developing baby needs extra red blood cells in order to absorb enough oxygen from the placenta. After birth these extra red blood cells are no longer needed. The excess blood cells are broken down releasing biliverdin (a green pigment) which is then changed into bilirubin (a brownish yellow pigment). The bilirubin is made water soluble (conjugated bilirubin) in the baby’s liver so that it can be excreted via the poops (stools). The yellow skin colour of jaundice appears when the baby’s immature liver struggles to process the temporary build up of bilirubin.
A little jaundice is normal
Bilirubin levels usually peak around the third to fifth day and then gradually fall and most newborn jaundice doesn’t need treatment.2 After about two weeks after birth, less bilirubin is produced and jaundice often disappears naturally at this point (NHS, 2022).
Protective effects
Normal newborn jaundice may be beneficial to the baby as biliverdin is thought to have anti-inflammatory properties3 and bilirubin may have anti-oxidant properties (protects against cell damage)4. There is also research suggesting jaundice could protect babies from sepsis (a bacterial infection).56 In many exclusively breastfed babies jaundice can last for many weeks without the levels of bilirubin being harmful—this is known as breast milk jaundice see Jaundice in Breastfeeding Babies.
Too much bilirubin can be harmful
If bilirubin levels continue to rise however, this can cause a baby to be sleepy and not feed well which in turn worsens the jaundice. If there are concerns about a baby, the levels of bilirubin will be checked by a blood test or transcutaneous bilirubinometry since visual observations can vary with different lighting and skin tones. Too much bilirubin over a certain threshold acts as a toxin that could cause permanent brain injury. In rare cases, high levels can lead to acute bilirubin encephalopathy (ABE) or kernicterus.7
Risk factors for jaundice
There are a number of factors and medical conditions that can increase the risk of exaggerated jaundice including a baby who is not getting enough milk, a premature baby, babies with blood group incompatibility, and babies with infections or metabolic disorders. Flaherman and Kair8 list the risk factors that increase the likelihood of exaggerated jaundice to include babies who:
- Are not getting enough milk—for example if there are problems with breastfeeding (sometimes called starvation jaundice or not enough breast milk jaundice). See Jaundice in Breastfeeding Babies for more information.
- Have a blood group incompatibility, most commonly Rhesus or ABO incompatibility9
- Have red blood cell abnormalities eg glucose-6-phosphate-dehydrogenase (G6PD) deficiency (a hereditary enzyme deficiency more common in those from mediterranean countries and south east Asia)
- Have birth trauma such as serious bruising e.g. from forceps or ventouse delivery, or have a cephalohematoma
- Are born too early (premature babies)
- Are poorly with an infection eg urinary tract infection or sepsis
- Have metabolic disorders such as hypothyroidism, galactosemia, Gilbert’s Syndrome or Crigler-Najjar syndrome (Wambach and Spencer, 2021 p 358)
- Are genetically susceptible eg Asians, Europeans and Japanese have an inherited difficulty with bilirubin processing (Wambach and Spencer 2021, p 359)
- Have mothers with diabetes.
For further information on risk factors see Nice Guidelines 2025, and Academy of Breastfeeding Medicine Protocol (ABM), 2017. Whatever the cause of the jaundice, bilirubin levels will be higher if the baby is not feeding well. Treatments to reduce bilirubin levels usually involve phototherapy and supplementation with more milk when needed, see Treatment for Jaundice for more information.
What are the symptoms of jaundice?
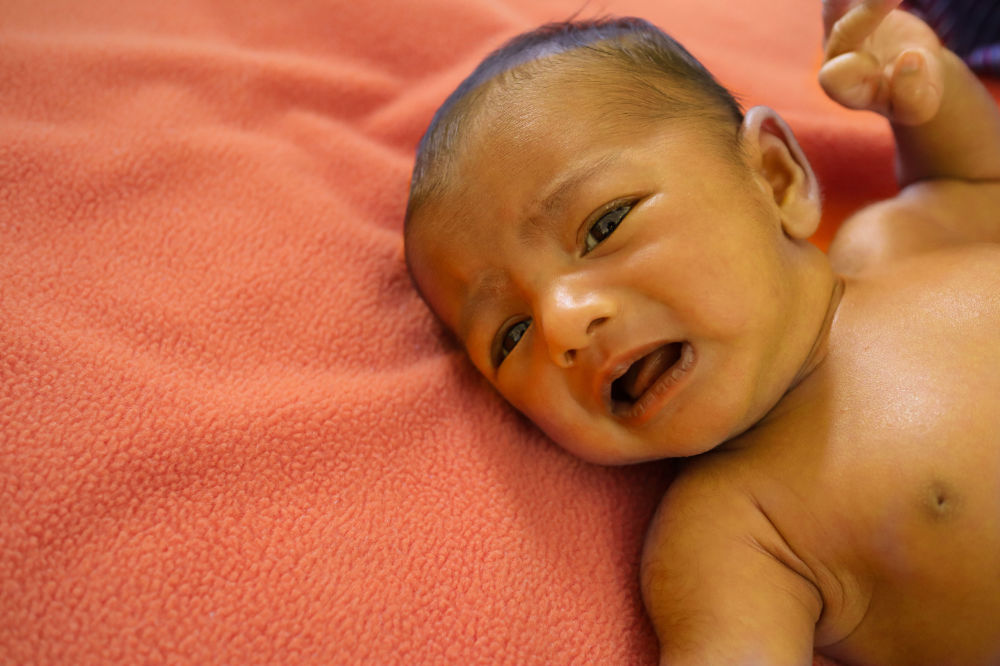
Yellowing of the skin
The yellow skin colour of jaundice starts at the head and moves down the body towards legs and feet as the levels rise and the condition worsens. Jaundice below the level of the tummy button or on the palms of hands and soles of feet should always be reported immediately to a doctor. Any yellowing of skin and whites of the eyes in your baby’s first 24 hours of life is also a particular concern.
A video from Global Health Media Project; Newborn Care Series: Jaundice (linked below) explains how to check for jaundice (in natural daylight) by applying finger tip pressure to the skin and then checking for a yellow colour when the pressure is released. Bear in mind that checking for jaundice by observing the progress of the yellow colour in your baby’s skin from head to toe is not as reliable as medical testing. Visual observations can vary with artificial lighting and different skin tones. Wambach and Spencer state that visual assessment is unreliable and inaccurate particularly in babies with darker skin tones (Wambach and Spencer, 2021 p 358). A health professional will usually check bilirubin levels by a blood test or transcutaneous bilirubinometry, see Treatment for Jaundice for more information.
Pale coloured poop
When breastfeeding is going well, normal newborn baby poop goes through distinct colour changes in the first five days (black, dark green, khaki, brown and finally yellow) and usually remains mustard/yellow after day five. Poop that is pale or chalky white should always be reported to your health professional. You can download the Children’s Liver Disease Foundation’s leaflet Jaundice in the New Born Baby (pdf) for further information and a stool colour guide.
Sleepy baby
Jaundice may make a baby sleepy and unable to feed well, they may have a high pitched cry or seem limp and floppy.
Dark urine
Urine should be pale coloured or colourless, dark urine could be a symptom of jaundice.

Summary
A certain level of newborn jaundice is normal due to a break down of excess red blood cells releasing the yellow pigment bilirubin. If the levels of bilirubin get too high however, this could be dangerous for your baby. A number of risk factors can cause problematic jaundice including not getting enough breast milk. Symptoms include a yellowing of the skin which progresses down the baby’s body from head to toe, sleepy behaviour and poor feeding, pale coloured poops and dark coloured urine. Seek medical attention if you have any concerns and especially if you see:
- Jaundice (yellowing of skin and whites of the eyes) in your baby’s first 24 hours
- Jaundice below the tummy button and on palms of hands and soles of feet
- Jaundice in conjunction with the danger signs of poor feeding, lethargy, convulsions
- Very pale or chalky white poop or stools that appear fatty
- Dark urine
For more information about the different types of jaundice while breastfeeding see Jaundice in Breastfeeding Babies and for information about treatments see Treatment for Jaundice.