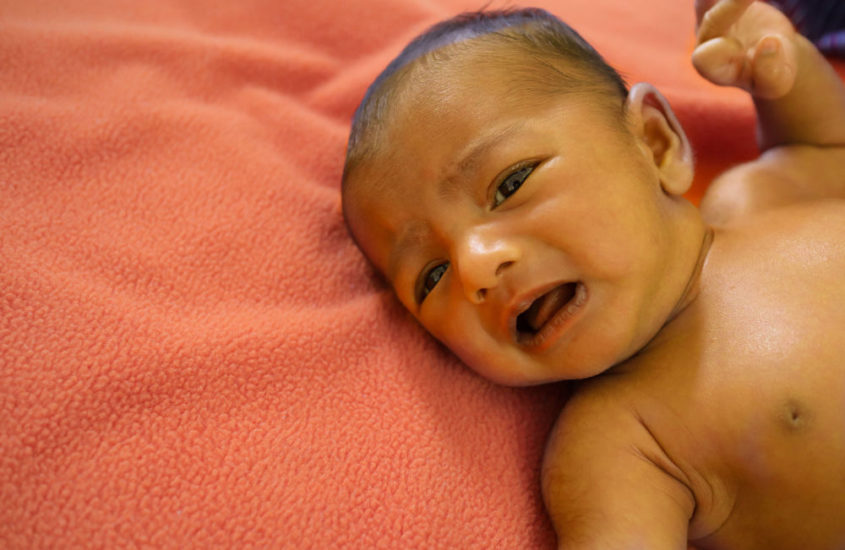
The yellowing of the skin and whites of the eyes sometimes seen in a newborn baby is known as jaundice. It happens when excess blood cells that the baby no longer needs after birth are broken down, and a brownish yellow pigment called bilirubin is released.
This article discusses how breastfeeding can affect jaundice and is a companion article to Causes and Symptoms of Jaundice and Treatment for Jaundice. Breastfeeding can almost always continue without interruption.
Newborn jaundice
Newborn jaundice is a normal process—however if bilirubin levels continue to rise past a certain threshold it could be harmful to your baby and may require treatment. A yellowing of the skin progresses down the baby’s body from head to toe and can be accompanied by sleepy behaviour, poor feeding, pale coloured poos and dark coloured urine. Always check with a health professional if you have any concerns about jaundice and for more reading on jaundice symptoms see Causes and Symptoms of Jaundice.
Types of jaundice in breastfeeding babies
There are different types of jaundice and these include:
- Normal newborn jaundice—a normal event for all newborn babies however they are fed
- Breast milk jaundice—a prolonged form of normal jaundice that may last for many weeks in breastfed babies but is not harmful
- Starvation jaundice—jaundice caused by not getting enough milk as might happen when there are difficulties breastfeeding or a mother’s milk supply is late coming in
- Pathological jaundice—certain medical conditions may cause or increase jaundice.
Combinations of these types of jaundice may occur at the same time which could contribute to higher levels of bilirubin. Whatever the cause, it is helpful to make sure breastfeeding is going well and the baby is getting plenty of milk as this can improve symptoms.1
#1 Normal newborn jaundice
Also known as physiological (normal functioning) jaundice, physiologic hyperbilirubinemia or icterus.
It is normal for a newborn baby’s bilirubin levels to rise after birth and then drop again during the first two weeks of life. In the first five days the levels of bilirubin in formula fed babies are the same as well-fed breastfed babies 2 Author Nancy Mohrbacher says:
In most newborns, jaundice is temporary, resolves on its own, and does not require treatment. Bilirubin levels in the full-term, healthy baby usually peak between the third and fifth days of life at less than 12mg/dl (204 µmol/L), and rarely go higher than 15mg/dl (255 µmol/L)
#2 Breast milk or late-onset jaundice
Also known as prolonged physiological jaundice.
In some exclusively breastfed babies jaundice can last for many weeks. Although there is the typical yellowing of the skin, the baby is well, gaining weight and has no underlying disorders. Monitoring from the health care team indicates the levels of bilirubin are not harmful. When jaundice appears after the fifth day of life in healthy, thriving breastfed babies it is known as breast milk jaundice.3 The Academy of Breastfeeding Medicine says it may take two to three months for bilirubin levels to fall4. In comparison, jaundice in full term formula fed babies tends to last seven to ten days.
The exact reason for prolonged jaundice is not clear but may be caused by factors in mature breast milk that promote the reabsorption of bilirubin in the intestine (called enterohepatic circulation). Bilirubin may have some protective effects for the newborn baby, see Causes and Symptoms of Jaundice for more information.
Continue breastfeeding
Your health professionals will keep an eye on bilirubin levels while breastfeeding continues and may carry out tests to rule out more serious causes of jaundice. They will advise if any treatment is needed should levels rise towards a certain threshold. Contacting an IBCLC lactation consultant if there are any problems with breastfeeding or milk supply, will help avoid the possibility of getting starvation jaundice (see below) and breast milk jaundice at the same time. The following paper from Gartner discusses the levels of bilirubin found in breast milk jaundice in a full term baby and see Jaundice in Newborn Babies Under 28 Days for guidance from NICE (National Institute for Health and Care Excellence).
The full-term infant with breastmilk jaundice of less than 340 µM/L (20 mg/dl ) requires no intervention, and breastfeeding should be continued without interruption. For those full-term, healthy infants with breastmilk jaundice and serum bilirubin levels between 340 and 425 µM/L (20 and 25 mg/dl ), closer observation of bilirubin concentrations is indicated. Some clinicians may wish to observe, whereas others may choose to complement breastfeeding with formula for 24 to 48 hours, which will reduce intestinal bilirubin absorption, or initiation of phototherapy. When serum bilirubin concentrations rise toward 425 µM/L (25 mg/dl), the use of phototherapy while continuing breastfeeding, or the interruption of breastfeeding for 24 hours, substituting formula, may be indicated.
If a baby is poorly or premature, the safe level for bilirubin may be lower and will require closer monitoring.
Carefully monitored breast milk jaundice is unlikely to cause harm and the jaundice will gradually fade without treatment. However, prolonged jaundice can be an indication of serious liver disease or involve some other cause (Gartner, 2001).
Split bilirubin blood test
The Children’s Liver Disease Foundation (CLDF) describe a test called the split bilirubin blood test which can identify liver disease:
Quite frequently parents are reassured that the cause of prolonged jaundice is breast milk jaundice without testing. The majority of babies will have breast milk jaundice but very few will have liver-related jaundice — or even both. However, it is important that a diagnosis of breast milk jaundice is made after a split bilirubin test is carried out and not before.
#3 Starvation jaundice or breastfeeding jaundice
Also known as breast non-feeding jaundice, suboptimal intake jaundice, or not enough breast milk jaundice.
Breastfeeding or starvation jaundice can happen in the first few days of life or it can occur later in the newborn period. This is caused by baby not having enough milk and it is the baby equivalent of adult starvation jaundice (Wambach and Spencer, 2021). Any problems breastfeeding, or a delay in the mother’s milk supply “coming in” may increase reabsorption of bilirubin in the intestines and subsequent jaundice (ABM, 2017). A baby may have a combination of breast milk jaundice and starvation jaundice at the same time (Gartner 2001) which highlights the importance of getting breastfeeding off to a good start from birth—see below for further information.
#4 Abnormal or pathologic jaundice
A number of medical conditions can cause abnormal jaundice however baby is fed (see risk factors below). This type of jaundice usually appears within the first 24 hours after birth. It can also be combined with breast milk jaundice and/or starvation jaundice so, as above, it is still important to get feeding off to a good start with help from your board certified lactation consultant and see ABM Clinical Protocol #22, 2017.
Risk factors
Some babies are more at risk of jaundice than others. There is a list of risk factors in Causes and Symptoms of Jaundice and includes:
- Babies not feeding well
- Babies with a blood group incompatibility
- Babies born too early
- Babies who have infections
- Babies with metabolic disorders or conditions
- Babies with bruising
- Babies of East Asian ethnicity
- Babies whose mothers have diabetes
Blood Incompatibility Jaundice
One of the risk factors for abnormal jaundice is if there are certain incompatible blood types between mother and baby. Derby National Health Service (NHS) in the United Kingdom have a handout explaining more:
Rh incompatibility
If the mother’s blood group is negative and the baby’s blood group is positive, antibodies may be made by the mother to protect her against what the body recognises as different cells. These antibodies invade the baby’s blood stream and surround his/her red blood cells causing them to break down. This is called ‘Haemolytic Disease of the Newborn’. It is usually prevented by screening during pregnancy and by the mother having an ‘Anti D’ injection to prevent the antibodies being produced.
ABO incompatibility
Different blood groups already have antibodies present. This means that if the mother’s and the baby’s blood group are different and they become mixed for some reason, the mother’s antibodies will break down the baby’s red blood cells, as happens with Rh incompatibility. Both of the above conditions are usually diagnosed quickly, as your baby will become jaundiced within 24 hours of birth.
For further information on risk factors and guidance see Nice Guidelines 31 October 2023, and Academy of Breastfeeding Medicine Protocol (ABM), 2017.
Can I breastfeed when my baby has jaundice?
A baby with newborn jaundice can usually continue to breastfeed alongside any medical treatments or additional supplements that may be needed, except in rare cases.56 It is important to get successful breastfeeding established early to avoid high levels of bilirubin that might require treatment (ABM, 2017).

Get breastfeeding off to a good start
Comprehensive ideas to minimise jaundice are listed in the Jaundice protocol from the Academy of Breastfeeding Medicine. They include; starting breastfeeding as soon as possible (within the first hour), exclusive and frequent breastfeeding, knowing when to spot early feeding cues, getting positioning and latch as good as possible, being vigilant for poor milk transfer, signs of dehydration, high weight loss, and identifying babies at risk. Other tips include avoiding mother-baby separation, using both breasts per feed, breast compression, skin-to-skin and avoiding using a dummy (pacifier). An IBCLC lactation consultant can be an excellent source of help and support and see our articles:
- A Good Start to Breastfeeding
- Breastfeeding Tips for Newborns
- Is My Baby Getting Enough Milk?
- Why Hire an IBCLC?
If baby isn’t feeding well
A poorly baby, low weight baby, premature baby or one with a poor suck/latch may be unable to breastfeed effectively at first. Jaundice can cause babies to become sleepy and to want to feed less often. In these situations hand expressing colostrum and then pumping will help a mother protect her milk supply and provide plenty of supplements to feed her baby if he is unable to latch properly and get the milk directly. The supplements can be fed by cup (baby must be alert and awake), syringe, or bottle to ensure the baby is getting plenty of calories. If a mother can’t express enough milk then banked donor milk or formula milk may be necessary for a time. Useful articles include:
- How to Make More Breast Milk
- How Can I Pump More Breast Milk
- Breastfeeding a Sleepy Baby
- When Baby Won’t Breastfeed
Treating jaundice
When bilirubin levels are too high treatments usually involve phototherapy and supplementation with additional milk as needed. For information about treatment for jaundice and links to clinical protocols see Treatment for Jaundice.
Summary
There are several different types of jaundice; normal newborn jaundice, breast milk jaundice, starvation jaundice, and pathological jaundice. More than one type of jaundice could be present at the same time. Breastfeeding doesn’t cause jaundice but poor feeding and not getting enough breast milk is a risk factor for high levels of bilirubin. Getting breastfeeding off to a good start and ensuring your baby is well fed can help avoid high bilirubin levels.