How often should a mother pump to build up her milk supply and how long for? When is the best time to pump when she is also breastfeeding? Are there any tricks to get more milk in less time? What is the best breast pump to use? This article shares tips to increase milk supply when pumping and is a companion article to Do I Need a Breast Pump?, Exclusively Pumping Breast Milk and How to Make More Breast Milk.
How often should I pump?
Breast milk is made by supply and demand. The faster milk is demanded from the breast by either a nursing baby, hand expression or a breast pump, the more quickly breast milk will be made in the breast to meet that demand. It follows that a higher total number of pumping sessions per day is more beneficial for supply than fewer sessions further apart. Exactly how often to pump depends on why you are pumping and how much breast milk is needed—pumping excessively if it isn’t needed could contribute to engorgement (breast inflammation) and/or oversupply of milk.
Reasons to pump include:
- Baby not breastfeeding. If baby is not breastfeeding at all in the early days or weeks it is important to pump as often as a baby would normally feed to stimulate the breasts to build a full milk supply. This will mean aiming for at least eight to ten pumping sessions per 24 hour period at first. Some mothers may prefer to pump regularly every two to three hours and others might find it easier to pump more often at certain times of the day to meet the same total. It is recommended to avoid long stretches of five or six hours between pumping sessions and to try to pump at least once during the night.1
- Baby needs more milk. If your baby is breastfeeding but needs more milk because of low milk supply, low weight gain, or difficulties breastfeeding—pumping and/or hand expressing after as many breastfeeds as possible can help to maximise your milk production by demanding more milk from the breast. Pumping six to eight times per day is a good goal in the first few weeks or as many times as you can manage. If there isn’t much milk straight after a breastfeed, you may prefer to try pumping about an hour later/between feeds (see next section). Any pumped milk can be used to top your baby up. It can be helpful to work with a breastfeeding specialist to identify the reasons for low milk supply and for help with any other difficulties such as the way your baby attaches to the breast (latches). See also How to Make More Breast Milk.
- Going back to work. If you are pumping to stockpile breast milk for a separation or ready for going back to work, you could start pumping once or twice a day, according to your needs, and begin to store a little each day. Mothers often have more milk early in the morning so this may be a good time to pump. Some mothers may choose to only pump one breast to be sure there is plenty of milk available in the other breast should their baby wake for their next feed straight after a pumping session. Once you are at work, the milk pumped for your baby when you are away from each other can be stored in the fridge for use the next working day.
- Exclusively pumping. If a mother is exclusively pumping and not breastfeeding long term, once she has reached full milk production she may be able to adjust the number of pumping sessions to maintain production according to her own milk storage capacity. For some mothers this might be four or five times a day while for others it might be nine or ten. For more information about pumping for a baby who isn’t breastfed directly see Exclusively Pumping Breast Milk.
When should I pump?
If a baby is not latching then a mother can pump when convenient with the goal of trying to fit in as many pumping sessions as possible to mimic the normal feeding pattern of a newborn baby (eight to ten feeds per day). However if a baby is also breastfeeding directly it can be difficult to know when is the best time to pump or even to find time to pump at all. Strategies include:
- Pump straight after breastfeeds. Ensuring the breasts are thoroughly emptied of milk (drained) by pumping straight after a breastfeed will help the supply and demand process by increasing milk production even though a mother may not physically pump very much milk at this time. Pumping after a breastfeed is often suggested as part of a care plan when supplementing a low gain baby. See Supplementing an Underweight Baby for more information about combining breastfeeding, pumping and supplementing.
- Pump between feeds. Another strategy is to pump between breastfeeds. Pumping an hour after a breastfeed is likely to yield more milk to give your baby as a top up and will help increase milk production. However there is a chance that a baby may be ready for their next feed while you’re pumping/just after you have pumped which may mean there is less milk available for that feed.
How long should I pump?
When increasing a milk supply by pumping, the goal is to pump long enough to efficiently remove milk from all areas of the breast and stimulate the milk making glands to increase production. A lactating breast is never truly empty so in practice this means removing or “draining” most of the available milk. The ideal pumping time to achieve this will vary for different women according to:
- Breast storage capacity. The amount of milk a breast can store at one time is referred to as breast storage capacity. Mothers with a smaller breast storage capacity will need to pump for a shorter time more frequently compared to mothers who have a larger storage capacity.
- Rate of milk flow/breast pump. How quickly a mother’s milk flows, the efficiency of the breast pump (manual, single electric or a double pump pumping both breasts at the same time) and whether the pump flange is the right size will affect the time needed to drain individual breasts thoroughly.
- The reason for pumping. Pumping to increase milk supply or exclusively express may require longer pumping sessions than expressing milk for an occasional missed feed, or expressing enough milk until the breasts feel soft and comfortable if you’re engorged.
- Pumping vs breastfeeding. If the pumping session follows an efficient breastfeed there will be less milk to remove from the breast. When trying to increase a milk supply, authors Marasco and West suggest pumping for at least 5-20 minutes after a breastfeed even if there isn’t any milk flowing during some of this time2
So how long is a reasonable guide?
One study of mothers of preterm babies found a double pumping session that incorporated massage (hands on pumping; see below) averaged 25 minutes with a range from 15 minutes for some mothers to 45 minutes for others.3 Lactation consultant Nancy Mohrbacher suggests pumping for twenty minutes as an initial guide and then adjusting the time pumped according to a mother’s milk flow: simply pumping for a longer or shorter time as needed to remove all the milk (Mohrbacher. 2020. p. 490).
How much milk should I pump?
- If you’re pumping to increase milk supply after breastfeeding your baby, the volume of milk produced at first may be quite small and it may sometimes help to view pumping as a way to stimulate the milk making glands to increase production without an expectation of a set volume.
- If you’re pumping for a replacement feed this could vary widely from 30ml to 120ml depending on your baby’s needs and how often they feed. A rough average guide to the daily volume of breast milk a baby takes from one month to six months of age is 750-1035 ml or 27-35 oz (Mohrbacher, 2020 p476) or an average 800 ml/day.4 If 800ml is divided by ten feeds this might make an expected volume of 80ml per feed—for a baby who tends to feed every two hours during the day with one longer break of four hours during the night. In practice this volume could be higher or lower for any individual baby.
- If you’re pumping to get top-up milk because your baby isn’t gaining much weight and needs more milk, the volume needed could vary widely. In this situation it is best to stay in close contact with your IBCLC and/or health professional to find the amount of milk you will need to keep your baby well fed, to see their weight increase and for help with the other issues that have led to the low weight gain. For much more information see Baby Not Gaining Weight and Supplementing an Underweight Baby.

How to pump more breast milk
#1 Pump more often
The more often the breasts are throughly drained the more milk will be made. If you’re not already pumping around eight or more times in 24 hours try increasing the number of pumping sessions. If you’re away from your baby, try to pump as often as baby would normally feed.
#2 Massage or “hands on pumping”
Massage or hands on pumping is a technique that is said to substantially increase the amount of milk expressed with a breast pump. Hands on pumping involves using your hands to gently massage and compress the breasts before and during pumping. One study showed a daily increase of breast milk volume of almost 50% with hands on pumping5 and an increase in the calorie content of the pumped milk6. Jane Morton MD from Stanford School of Medicine has developed a helpful Hands on Pumping video (see 5:15) and Exclusively Pumping Breast Milk also explains the technique.
Caution. It is important to use a light sweeping touch equivalent to stroking a pet or applying ointment to your body if using breast massage. Deep massage can cause bruising or breast inflammation and is not recommended.78

#3 Hand expressing and pumping
Combining hand expressing with hands on pumping can help to produce more milk particularly in the first few days after birth before milk volume increases and when using hand expressing techniques straight after a hands on pumping session.9 See Hand Expressing Breast Milk for tips and videos.
#4 Double pumping
Double pumping (pumping both breasts at the same time) saves time and can help produce more milk1011 although it is not essential for good results12. Some single pumps can be converted into doubles at a later date. For hands on pumping and double pumping at the same time you can buy hands free double pumping bustiers. If you’re single pumping, alternate between left and right breasts every five minutes and repeat.
#5 Try a different pump or flange size
- Flange fit. How the part of the pump that is held next to the breast (the flange) fits around your nipple is important to the success of your pumping session. See “How to choose a breast pump,” “How to use a breast pump” and “Breast pump flange fit” below for much more information.
- Different pumps for different mothers. Sometimes a breast pump might be faulty and not working properly, particularly a second hand pump. Or sometimes a particular brand just might not work well for an individual mother and she may have more success with a different pump. Pump suction should not be painful.
#6 Pump at night
Try pumping at night especially if you happen to be awake anyway, because prolactin levels (an important hormone in milk production) are higher at night. If you usually breastfeed at night, that will also help to stimulate milk production.
#7 Power pumping
Power pumping is a short-term technique made popular by lactation consultant Cathy Watson Genna and described in the book Making More Milk (2020). Although there are many variations possible, the technique aims to mimic a baby cluster feeding which can boost milk production. The method in the book involves setting up a pump in a handy, comfortable spot and every time a mother passes by as she moves around the house, she pumps for five or ten minutes as often as every 45-60 minutes. The goal is to pump at least ten times each day for two or three days and then return to the usual pumping schedule. The technique suggests parents of healthy full-term babies can leave the pump set up and only refrigerate milk or wash equipment every four hours depending on the temperature of the room (Marasco and West. 2020). However official guidance recommends that equipment is washed after each use.1314 See How Long Does Breast Milk Last? for more information.
#8 Skin-to-skin
Spending time in skin-to-skin contact with your baby can help boost oxytocin, one of the hormones involved in milk production and studies have found mothers can pump more milk after skin-to-skin contact.1516 Some mothers find holding their baby while they pump can help increase their pumping output. If your baby isn’t available, photographs of your baby or an item of clothing that smells of your baby can help oxytocin to flow.
#9 Pumping on one breast while baby breastfeeds on the other
This works well for some mothers who find it difficult to let-down to the pump.
#10 Warmth
One study involving mothers pumping for premature babies found that warming one breast with a warmed cloth for twenty minutes before pumping produced significantly more milk than the unwarmed breast.17 Another study found that using a warm breastshield improved the efficiency of milk removal.18
#11 Lubrication
Lubrication inside the pump flange and/or on the breast can make pumping more comfortable by reducing friction. Mothers have used oils (e.g. coconut oil or olive oil), breast milk or lanolin as lubricants. Marasco and West state that with the correct sized pump flange, lubrication should not be needed (Marasco and West. 2020.p 196)—it is important to check the flange is centred on the nipple, and you are using the pump correctly (see below) but a little lubrication may still be helpful for some mothers.

#12 Music and relaxation
Studies have found that mothers who listened to guided relaxation recordings, music and looked at baby photos while they pumped, could pump much more breast milk.19202122
#13 Pumping rituals
Pumping with the same pre pumping rituals can help some mothers to relax and let-down their milk. This can be important for mothers who find it difficult to release milk to a pump. Nancy Mohrbacher suggests wrapping a blanket around the shoulders for warmth, using gentle massage and spending five minutes using guided relaxation techniques before pumping. (Mohrbacher, 2020 p 480) For further tips to help condition the let-down reflex see Exclusively Pumping Breast Milk.
#14 Cover the collection bottle
Some mothers find watching the collection bottles to see how much milk they are pumping at each session is quite stressful. Covering the pumping bottle with a sock or mitten can take the focus off the volume collected and, if it helps a mother to feel more relaxed as she pumps, she may pump more milk as a result.
#15 Record milk volumes
Keeping a record of the milk pumped can encourage some mothers when they see a gradual increase over time and realise their efforts are being rewarded.

How to choose a breast pump
Different pumps suit different mothers and one type isn’t necessarily better than another for an individual mother (Mohrbacher, 2020 p 487; Marasco & West, 2020 p 192). Do I Need a Breast Pump? describes the types available including manual pumps (hand operated), silicone pumps, electric pumps and hospital grade pumps (expensive multi-user pumps used in hospitals). An electric pump will usually be much more efficient than a manual one and hospital grade pumps will be better still. But there can be exceptions to every rule and some mothers may even find hand expressing works better than pumping for them. Tips for choosing a pump include:
- Look for a pump with multiple settings for speed and suction to give you more comfort and control and to mimic a baby’s sucking pattern. Some breast pumps can generate unsafe vacuum levels or maintain a vacuum for too long. Pumping should not hurt and pumping with a suction that is too high can inhibit milk release (Mohrbacher, 2020 p 490)
- Consider whether you want a single pump or a double pump. A double pump allows you to pump both breasts simultaneously which can save time but some mothers find it easier to pump each breast separately.
- Look for a choice of flange size. The part of the pump that is held to the breast has various names with different pump manufacturers such as breast shield (Medela), breast shell (Ardo), funnel (Ameda) or flange. Look for a pump with different sized flanges because nipples and breasts are not all the same size and the right fit is important for your comfort levels (pumping should not hurt!)—see “Breast pump flange fit” below.
- Availability of replacement parts. Consider whether a battery back up option would be useful in addition to mains operated.
- Check reviews online from other women who have tried them before buying a pump. However bear in mind that just because one pump suited a colleague, friend or relative doesn’t mean that it will be perfect for you.
- Hospital grade pumps may be available to borrow from your maternity hospital or for short-term hire from major pump manufacturers in your country e.g. contact Ardo, or Medela in the UK.
- Second hand pumps may not work efficiently and may have hygiene concerns23. The Womanly Art of Breastfeeding explains:
…consumer-grade pumps aren’t built to last much more than a year or so, the average length of time that a mother might be pumping for one baby. When they start to wear out, they don’t just suddenly stop working. The suction and cycling mechanisms veeerrry slowly break down, and eventually you realise you aren’t pumping as much milk and the suction doesn’t feel as strong (or is too strong). Consumer-grade pumps aren’t closed system like rental-grade pumps, so milk and moisture may have entered the mechanical parts, where bacteria, mould, and viruses can grow.
Breast pump flange fit
Using a breast pump shouldn’t hurt, but if the flange doesn’t fit correctly (or the vacuum is too high), pain and friction can result in sore nipples and may negatively affect milk flow. The opening where the nipple sits, is sometimes referred to as the nipple tunnel. The nipple should be positioned in the centre of the tunnel. Lactation consultants Marasco and West say that although the nipple may touch the sides of the tunnel, during pumping the nipple should move freely and the areola (the area of darker skin around the nipple) will move slightly as well (Marasco and West. 2020. 196).
- If the nipple tunnel is too large, too much areola may be pulled into the tunnel to rub along the sides, causing swelling and redness of the areola and nipple and compromise milk flow (Marasco & West 2020 p 196).
- If the nipple tunnel is too small the nipple may rub along its sides or get wedged, this can cause cracking at the base of the nipple or abrasions on the nipple tip24 or compress milk ducts and slow milk flow (Marasco & West 2020 p 196).
- A different flange size may be needed for each breast. Regular pumping (and breastfeeding) may also change nipple length and diameter so that a different sized shield may be needed over time (Mohrbacher 2020 p 477).
Getting the right fit
According to some authors, in addition to extending in length during pumping, nipples can swell (increase in size) as much as 3-4mm diameter during pumping (Wilson-Clay & Hoover. 2017 p 82). Indeed, some pump manufacturers such as Ardo or Medela’s guide to getting the right flange fit recommend choosing a flange that is 4mm (Ardo) or 5/6mm (Medela) wider than the diameter of the nipple at rest, presumably to accommodate this degree of swelling. However, in the 2022 Gold Keynote Presentation Fitting Flanges for Pumping: Rethinking Sizes and Materials, Jeanette Mesite Frem IBCLC shares her experience that when a nipple tunnel is too large, it can cause swelling of the areola and nipple, whereas in most cases a closer fit will not lead to nipples swelling.
Although mothers can measure their nipples as an initial guide (Pumpables has a printable nipple ruler), Jeanette advocates for trying a range of flange sizes to see what feels comfortable and gives the best milk yield. She has produced The Flange Fits™ Guide below reproduced courtesy of Babies in Common.
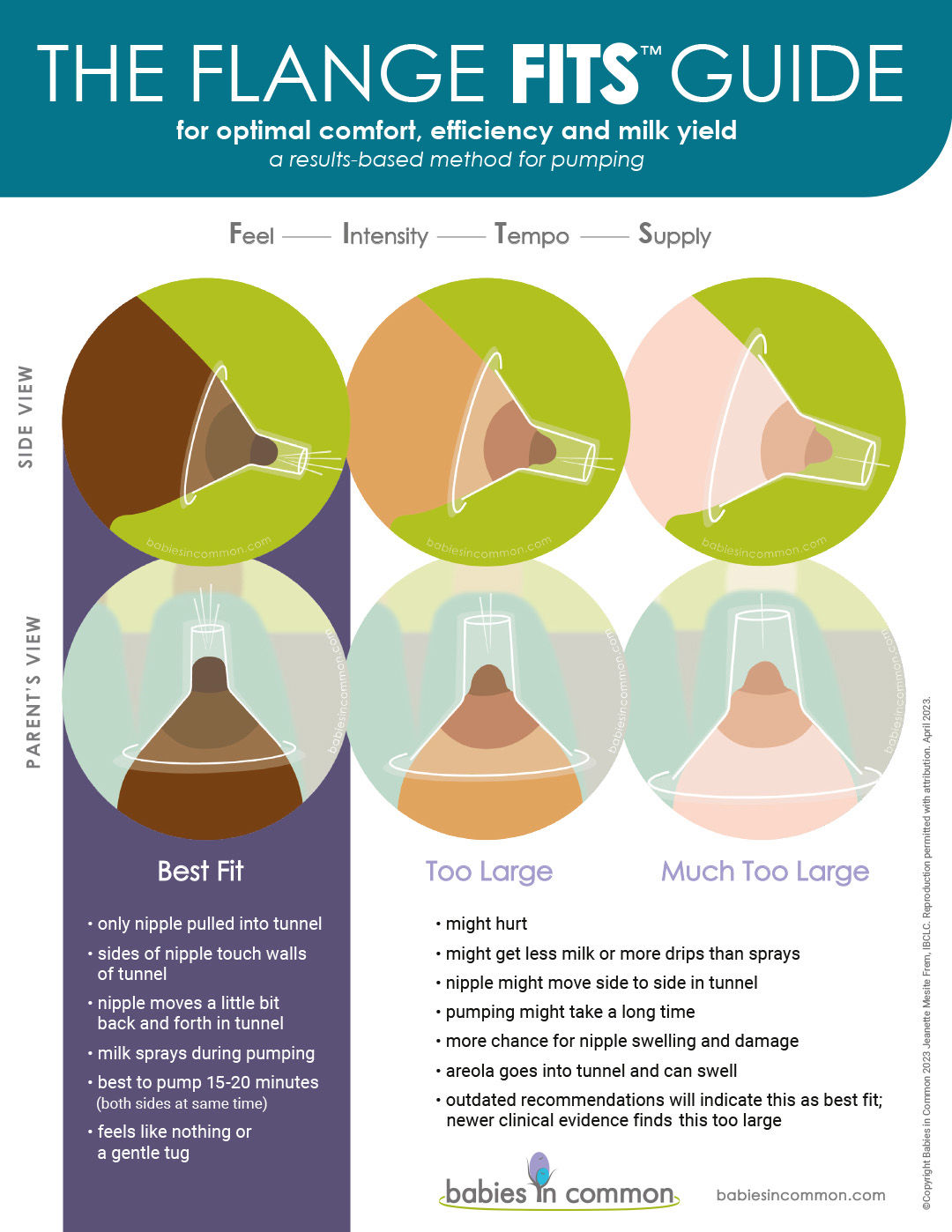
Flange sizes
Most pump companies offer a variety of flange sizes for example Ardo Breast Pumps (6 sizes: 18mm–36mm diameter), Ameda Breast Pumps (7 sizes: 21mm–36mm) and Medela (5 sizes: 21mm-36mm). Pumpables has a universal breast shield set in 6 sizes from 15mm to 29mm diameter and Maymom also offers a range of around 12 shield sizes compatible with several brands from 15mm to 36mm. Beaugen cushions can help to adjust the fit on standard flange sizes and are compatible with many brands of pump. Silicone inserts may not work as well as firm flanges for some mothers as they do not provide as much pressure to the breast tissue behind the nipple (Mesite Frem, 2022).
How to use breast pump settings
Variable settings on a pump include pump suction (vacuum) and pump speed (cycles per minute).
- Suction. It is usually recommended to use the highest completely comfortable vacuum setting (suction) that maintains milk flow (Mohrbacher, 2020 p490 & p906). If suction is high enough to cause pain or discomfort this could limit milk flow.
- Speed. By adjusting the speed (cycling) it is possible to mimic the faster sucks of a baby’s initial latch—which stimulate the let-down—followed by the deeper rhythmic suck later in the feed which keeps the milk flowing. You can also continue to adjust the speed during the feed to create several let-downs; i.e. increase the cycling speed when milk flow slows and adjust it down again when flow increases. Some pumps will do this automatically for you and may have a special “let-down” button or “power pumping” feature.
If you are single pumping (on one breast) switching between breasts several times will mimic switch nursing and stimulate let-downs. A little olive oil, coconut oil or lanolin smeared inside the flange and nipple tunnel can make pumping more comfortable if needed.
Cleaning breast pump parts
Pump parts that come into contact with breast milk should be cleaned after each use according to manufacturers’ instructions. Advice to sterilise equipment after each use or whether washing pump parts is sufficient varies between different regulatory bodies. The UK’s National Health Service recommends that all feeding equipment be sterilised after each use until a baby is one-year-old2526. The Centers for Disease Control and Prevention (CDC) have a fact sheet with tips for keeping pumping equipment clean, see How to Keep Your Breast Pump Kit Clean: The Essentials. The CDC recommend washing pump parts thoroughly after each use and sterilising equipment once a day particularly for babies under two months of age and vulnerable babies. However, the US Food and Drug Administration (FDA) and The Academy of Breastfeeding Medicine say that breast pump parts do not have to be sterilised:
Containers for human milk storage and breast pump milk collection kits must be completely dismantled, washed in hot soapy water and rinsed or washed in a dishwasher, and should always be thoroughly air dried or dried with paper towels. They do not need to be sterilized. If soap is not available, then boiling water is preferable.
All breast pump parts that come in contact with breast milk, such as bottles, valves and breast shields, should be cleaned after each use. It is not possible to completely sterilize breast pump parts at home, even if you boil them. However, sterilization is not necessary to keep these parts safe and sanitary. You can do that by thoroughly washing away germs and bacteria with liquid dishwashing soap and warm water.
Avoid harsh chemicals and abrasive scrubbing
Authors Wambach and Spencer 27 point out not to use harsh chemicals or abrasive scrubbing which could create small scratches to harbour bacteria or mould.
Tubing, diaphragms and pistons
Pump parts that don’t come in contact with milk such as tubes, and pistons are not meant to be sterilised and could melt under direct heat28 so follow manufacturer’s instructions carefully. If condensation develops in the tubing running the pump without the collection bottles and flanges attached can force air through the tubing to dry it (Wambach and Spencer 2020).
Other ways to increase milk supply
Pumping can be a great partner in the process to increase low milk supply, however not all mothers find pumping works well for them and there are many more ideas to try. Our article How to Make More Breast Milk discusses more ways to increase your milk supply and it is helpful to consult your breastfeeding specialist to unpick the reasons for low milk supply. With good positioning, some latching tips, breast compression, and by offering both breasts (and more!) you may be able to improve your supply with less need to pump.
Summary
There are several ways to help increase the amount of breast milk you can pump. Ideas include using breast massage while pumping, hand expressing after using a pump, pumping more frequently, choosing the right pump and pump flange, relaxation and pumping both breasts at the same time. A breastfeeding specialist can be a helpful partner when a mother needs to increase her milk supply.