Although babies have a strong instinct to breastfeed straight after birth, some babies may not seem interested in breastfeeding at first or may not seem able to attach to the breast. Some babies may still not be attaching to the breast (latching on) by the second or third day of life or even much longer. Why does this happen and how can a baby be helped to breastfeed? How often will a baby need to be fed if they can’t breastfeed? Should a mother start expressing her milk? When and how often? This article answers frequently asked questions when a newborn baby won’t breastfeed and is a companion article to How to Get Baby Back to Breast.
Why can’t my baby breastfeed?
There are several reasons why a newborn may not be able or ready to breastfeed at first. Despite this, babies have a strong instinct to latch for many weeks or months and most challenges can be overcome in time. Even if a mother has left the maternity hospital formula feeding her baby, and her baby is a few days or even weeks old; there is still plenty of time to get breastfeeding established. Possible reasons for not latching include:
- Birth drugs. Painkillers or other birth medications given to the mother during labour may make a baby very sleepy and/or less able to breastfeed. Over time the effects of any drugs will leave a baby’s system.
- A difficult birth. An instrumental birth (forceps or ventouse) or a birth injury may leave a baby feeling uncomfortable or in pain. These babies may need more time and support to get breastfeeding established.
- Positioning. The way a baby is held to the breast can often make a big difference to how easily they can use their feeding reflexes to latch on. See Breastfeeding Positions for Newborns, Breastfeeding Videos and Latching Tips for ideas to help with positioning and attachment.
- Separation after birth. Separation between mother and baby after birth can interfere with a baby’s feeding instincts. However babies have a strong instinct to breastfeed once they are reunited with the breast, held in skin-to-skin contact and in helpful breastfeeding positions.
- Prematurity or immaturity. Some babies who are born early may not be ready to latch on or breastfeed yet. But with the right support, even tiny babies can often get the hang of breastfeeding see Breastfeeding a Premature Baby and Kangaroo Care for Your Premature Baby.
- Mucus and congestion. Some babies may have mucus congesting their airways after the birth and not seem interested in breastfeeding at first. This will resolve over time.
- Feeding aversion. If a breastfeeding helper or parent has repeatedly pushed a baby’s head into the breast to try and force them to breastfeed, the baby may come to associate breastfeeding with a scary or even painful experience. Refusing the breast due to a bad memory or painful association is sometimes called a feeding aversion. It’s important to handle a baby gently at the breast and to remember that if they could breastfeed they would do so. For ideas to overcome a feeding aversion see below and see How to Get Baby Back to Breast.
- Differences of anatomy. Sometimes a mother and baby may have anatomical challenges. For example some babies may struggle with a mother’s flat or inverted nipples, large breasts or large nipples or have their own unique anatomy such as a cleft lip or palate, a small chin, high muscle tone or a tongue-tie that makes breastfeeding more challenging. Breastfeeding support from a specialist can be invaluable to help with anatomical challenges as they will know a range of latching techniques and ideas to try for each situation.
- Allergies. In her book Breastfeeding Works! Even With Allergies author Robyn Noble notes that some babies born with food intolerances and allergies can seem incompetent at the breast.

When baby won’t breastfeed
Until your baby can latch and breastfeed, it is very important to keep expressing breast milk to stimulate your milk supply and to keep your baby (or babies) well fed. If breast milk isn’t removed from the breasts regularly a milk supply will begin to dry up. Until your baby can breastfeed:
- Express your breast milk regularly
- Keep your baby well fed
- Try lots of skin-to-skin contact to encourage your baby to breastfeed
- Find a breastfeeding specialist to support you
Some authors refer to this as the three keeps: keep milk flowing, keep baby fed, keep baby close.1
#1 Express breast milk regularly
The first days after birth are when the breasts gauge future milk production. The more often milk is removed at this time, the more likely there will continue to be plenty of milk for all your baby’s needs as they continue to grow. It is therefore very important to keep expressing breast milk regularly if a baby is unable to empty the breasts by suckling.
How can I express breast milk?
Colostrum can be thick and sticky and not much of it at first so it is usually easier to hand express this into a spoon, small cup or collect drops in a syringe, rather than use a breast pump. See Hand Expressing Breast Milk for help to do this. For ways to feed this milk to your baby see “How Should I Feed my Baby?” below.
When should I start hand expressing?
If your baby isn’t breastfeeding, the sooner you can start hand expressing the better. Hand expressing in the first hour after birth is ideal and is discussed in Stanford University’s video Successful Breastfeeding Begins at Birth.
How often should I express my breast milk?
Hand express and collect drops of colostrum as often as you can, at least every two hours during the day and every four hours at night. Or at least eight to twelve times in 24 hours. Once your milk volume increases sufficiently (“comes-in”) some mothers find a breast pump is more efficient than hand expression. Breast milk generally increases in volume around the second or third day after birth—but it may be later than this (see below). Pumping both breasts every two to three hours in the day and every four hours at night, will help remove as much milk as possible. Some mothers find using gentle breast massage and breast compression can help to express more milk. See What is Breast Compression? and How to Increase Milk Supply When Pumping for more information.
How long should I pump for?
How long to pump at each session is quite individual to each mother because a mother with a small breast storage capacity will need to pump for a shorter time and more frequently, compared to a mother who stores more milk at one time. The topic is discussed in more detail in the following article:
Nancy Mohrbacher [lactation consultant and author] suggests pumping for twenty minutes for a few sessions while observing milk flow and then adjusting the time pumped as required: simply pumping for a longer or shorter time as needed to remove all the milk (Mohrbacher, 2020. p 490). The goal is to establish a full milk supply (750-1035 ml per day) by 10-14 days after the birth. Once the goal is met, pumping length may return to 10-15 minutes for some mothers.
Which pump shall I use?
Some hospitals or pump manufacturers hire out “hospital grade” pumps which are very efficient breast pumps that are ideal to get your milk supply off to a good start. For more information about types of pump see How to Increase Milk Supply When Pumping and Do I Need a Breast Pump?
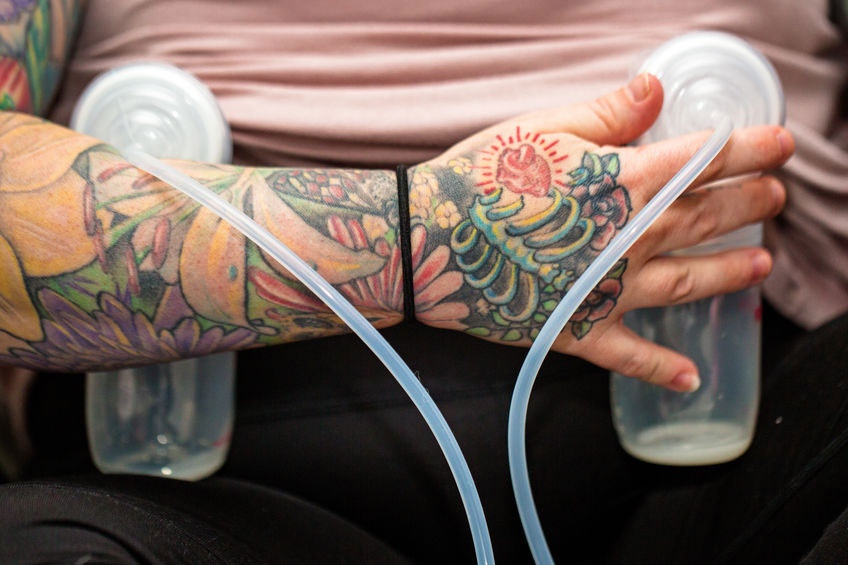
#2 Keep your baby well fed
A baby can’t be forced to breastfeed just because they are hungry. In fact if they are not getting the frequent small feeds they need, they will be more likely to keep falling asleep and not have enough energy to breastfeed well. Although newborn babies only need small volumes, they do need small amounts of milk frequently or they could become dehydrated.
How often should I feed my baby?
Whether or not they are breastfeeding yet, a newborn baby needs frequent feeds to keep them well fed and hydrated. Feed your baby at least every two to three hours in the day and every four hours in the night (the same as the pumping schedule above) and see How Often Should a Newborn Feed? for more information.
How much milk will my newborn baby need?
The amount of breast milk each baby needs to stay hydrated and satisfied is quite variable for each baby and their age and bodyweight. A baby needs enough milk to ensure they are pooing and weeing and gaining weight. After an initial weight loss typical of newborn babies in the first few days of life, breastfed babies will start gaining 30-40g (1oz) per day through the first three months. The following excerpt gives an example of volumes of breast milk (or formula if needed) that may be required every two to three hours:
- First 24 hours: 2-10ml breast milk per feed 2
- 24-48 hours: 5-15ml breast milk per feed (ABM, 2017)
- 48-72 hours: 15-30ml (o.5-1oz) breast milk per feed (ABM, 2017)
- 72-96 hours: 30-60ml (1-2oz) breast milk per feed (ABM, 2017)
- 2-3 weeks: 60-90ml+ (2-3oz+) breast milk per feed 3
- 1-6 months: 90-150ml (3-5oz) breast milk per feed or a total of 750-1035ml per day (25-35oz) (Mohrbacher, 2010)
What if my baby is very sleepy?
Try not to let your baby sleep too long as a newborn needs regular feeds. See Breastfeeding a Sleepy Baby for ideas to help wake a sleepy newborn.
How should I feed my baby?
Your baby can be fed all your expressed breast milk in a number of ways. Your maternity health professional will often advise you. Methods include: spoon, syringe, feeding cup, feeding tube alongside a finger (finger-feeding) or bottle and teat.
- Spoon and cup feeding. Spoon feeding and cup feeding can be useful for smaller volumes of expressed milk. Cup feeding is discussed in Cup Feeding a Newborn and both cup and spoon feeding are shown in this video from Global Health Media.
- Finger-feeding. For more information about finger feeding with a feeding tube see What is Finger Feeding?
- Bottle feeding. Avoiding using a bottle at first, may help to avoid nipple preference or nipple confusion; a situation where a baby starts to prefer the bottle teat and is less keen to breastfeed. However if you want to use a bottle see our Tips to Bottle Feed a Breastfed Baby and Best Bottle for a Breastfed Baby. which have lots of ideas to reduce the risk of bottle preference.
Is my baby getting enough milk?
There are lots of ways to tell if your baby is getting enough milk including weight gain, the colour and number of dirty nappies and whether they are swallowing milk and seem contented. See Is My Baby Getting Enough Milk? for much more information.
What if I don’t have enough milk?
If you’re still struggling to express any milk after the first few days, your milk supply may be delayed or occasionally a medical condition can cause low milk supply. Contact your breastfeeding specialist and see No Breast Milk After Delivery and Reasons for Low Milk Supply. Sometimes a baby may need some donor milk or commercial infant milk until your milk supply increases, your health professional will normally advise you when this is needed. Supplementing With Formula and How to Make More Breast Milk have more information
#3 Skin-to-skin contact
Skin-to-skin contact—with no clothes between you and baby—helps breastfeeding in lots of ways. See Why Skin-to-Skin? for a full discussion and for several videos of babies attaching to the breast all on their own. Skin-to-skin contact helps:
- Feeding reflexes. Skin-to-skin contact promotes your baby’s feeding reflexes to encourage instinctive breastfeeding. Covering a baby’s hands removes their sense of touch so remove any anti scratch mittens—see Scratch Mittens and Breastfeeding.
- Milk supply. Skin-to-skin contact promotes the release of the hormones needed for milk production.
- Comfort and calm a baby. Holding your baby comforts and calms him. Avoid passing your baby around friends and relatives so you can concentrate on getting breastfeeding established.
- Regulate body systems. Skin-to-skin contact helps to regulate a baby’s temperature, blood sugar levels, heart rate and breathing.
- Feeding cues. When baby is in close contact and held skin-to-skin, it is easier to see the signs that a baby is getting ready to feed (early feeding cues). This is a good time to try to breastfeed. Early feeding cues include a baby starting to fuss and fidget, searching for the breast with a wide open mouth and sucking on fists or fingers.
This short film from the Global Health Media Project shows how skin-to-skin contact helps babies use their feeding reflexes to latch to the breast straight after birth.
#4 Find a breastfeeding specialist
A breastfeeding specialist such as an International Board Certified Lactation Consultant (IBCLC) can be invaluable to help you and your baby start breastfeeding. The article Why Hire an IBCLC? on this website describes the different forms of support available. A breastfeeding specialist can help with:
- Positioning and attachment. A breastfeeding specialist will be able to suggest helpful positions and techniques to help your baby latch. They will have lots of experience of latching babies. Sometimes some experienced hands to guide you and your baby are all that are needed.
- Anatomical differences. A breastfeeding specialist will often know little tricks and tips to get around many challenges or know when to suggest a referral to a health professional for further assessment.
- Maximising milk supply. A breastfeeding specialist can help you devise the best plan to protect and maintain your milk supply.

Practical tips to help a baby breastfeed
Look for early feeding cues
It is helpful to practise breastfeeding as soon as a baby shows really early feeding cues such as starting to move in light sleep, moving their head from side-to-side to search with an open mouth, or sucking their fingers or fists. Crying is a late feeding cue and a baby is less able to organise themselves to breastfeed if they are crying and upset. A baby will have more energy to breastfeed and get less frustrated if they are not too hungry when they have a breastfeeding practice session.
Skin-to-skin contact, positioning and latch
As discussed above, holding your baby close in skin-to-skin contact can encourage your baby to latch on especially when you hold your baby in comfortable Breastfeeding Positions. Sometimes a baby can find it hard to grasp a mouthful of breast tissue along with the nipple. There are a number of ways to help with this eg supporting and shaping the breast—flattening it slightly—to fit your baby’s mouth can be helpful. Our article Latching Tips discusses latching step by step and an experienced breastfeeding supporter can help you in person.
Avoid pacifiers or dummies
A dummy can cause missed feeding cues and may interfere with getting breastfeeding established. See Pacifier, Dummy or Soother—Yes or No? for more reading about dummies.
Avoid bottle teats
If you have been using bottles for baby’s feeds and are not making progress towards breastfeeding, some mothers have found avoiding bottles (using a cup or finger feeding instead) encourages their baby to suckle since they no longer have their sucking needs met by an artificial teat.
Stay calm, be patient
It is natural to become very frustrated and upset if your baby can’t breastfeed and you don’t know how to help him. But a baby is very in tune with his mother and if he senses you are anxious whenever the breast appears, he will also feel more anxious. A baby will be more likely to focus on learning to breastfeed when they are calm, not too hungry and when they can sense you are calm too.

Nipple shield
In some situations a nipple shield may help a baby to latch and breastfeed e.g. if a mother has very flat nipples or a baby is premature. A nipple shield is a thin, flexible silicone cover with holes that is placed over your nipple during a breastfeed. Read more in Nipple Shields Good or Bad? and discuss using one with your breastfeeding helper.
Mammalian behaviours
The Womanly Art of Breastfeeding has another novel suggestion that may be helpful. They say:
All mammals lick their babies after birth, not only to clean them but also to stimulate their breathing, digestion, and neural responses. Licking is also used to show affection and enhance the sense of smell. Human mothers don’t typically think to do this, but some mothers have felt drawn to do it and their babies have responded surprisingly well.
Troubleshooting
Engorgement
Engorgement (when the breasts are very full with breast milk) can make latching more difficult see Engorged Breasts for tips to help with this including massage and something called reverse pressure softening which is a technique to temporarily push fluid away from behind the nipple to make latching easier.
Baby cries at the breast
If your baby cries as soon as they are held to the breast, they may be feeling frustrated with trying to breastfeed. They may associate breastfeeding attempts with being forced onto the breast, being hungry without reward or perhaps they sense that their mother is anxious about what is about to happen making them feel anxious too. If your baby has made this type of negative association (feeding aversion) try some of the following ideas to help them overcome this:
- Rescue your baby from their trauma rather than reinforcing their discomfort by repeatedly trying to breastfeed again and again against their wishes. Hold a distressed baby upright against your shoulder or between your breasts, walk around with them, talk or sing to them and calm them down before trying again.
- Stay calm. Try to stay calm, positive and patient at each breastfeeding practice session. Relax your shoulders and smile, talk to, sing or praise your baby.
- Not too hungry. Make sure to feed your baby a little expressed milk so they are not too hungry before they try to breastfeed.
- Happy place. Try to make the breast a happy relaxed place without pressure to latch in between feeding attempts or even take a short break from trying to breastfeed altogether—Time off to “Reboot” the Baby and Get Over Breast Distress discusses this.
- Try different positions. If breastfeeding isn’t working something may need to change. Try holding your baby in a different position that they don’t associate with previous breastfeeding attempts. If you usually use a cradle or cross cradle hold, try standing up to feed, lying down, reclining or rugby hold. See Breastfeeding Positions for Newborns for images of these positions.
- Seek support. Find a breastfeeding specialist to help you and see How to Get Baby Back to Breast for more ideas.
Baby prefers a bottle
If your baby has already become imprinted on a bottle teat as their preferred way of feeding see How to Get Baby Back to Breast, Tips to Bottle Feed a Breastfed Baby and Best Bottle for a Breastfed Baby.
Baby latches then pulls away/loses the latch
Occasionally a baby may latch on but then quickly let go of the breast again either before the milk flows or just after the milk begins to flow. Possibilities include:
- Nipple/breast shapes and sizes. Some babies may find challenges with certain shapes or sizes of nipple or breast which other babies would not find a problem. A very soft flat nipple can be harder for a baby to find and a baby may find it hard to keep hold of a heavy breast in their mouth. See Breastfeeding With Inverted Nipples and Flat Nipples and Breastfeeding With Large Breasts for breastfeeding tips and check in with your breastfeeding helper.
- Milk too slow. Some babies may need a little encouragement to stay at the breast to wait for the let-down (milk release). Hand expressing to ensure your milk is already flowing to instantly reward your baby’s latching attempts with milk can be helpful, and breast compressions and massage can keep the flow going until your baby realises how to control the flow.
- Milk too fast. Sometimes a baby can find it difficult to coordinate sucking with swallowing and breathing when milk begins to flow. And sometimes milk may be seen spurting and gushing like a hose causing a baby to cough and splutter. Most babies can cope better with the flow of milk if they are in a deep latch with plenty of breast tissue as well as the nipple in their mouth. See What is a Fast Let-Down? if you feel there is a challenge associated with flow.
- Pain or discomfort. A baby who is in pain from a difficult birth or discomfort from food intolerances may find it difficult to stay at the breast.
Problems once baby starts to breastfeed
Breastfeeding hurts
It will be a relief once your baby begins to latch on and stay at the breast but what if breastfeeding hurts? It will be tempting to put up with the pain because you’re just happy that baby is latched on. But doing so can quickly make your nipples sore and a baby will also find it more difficult to get the milk he needs. There are several reasons why feeding could be painful. It is usually because the baby doesn’t have enough breast tissue as well as the nipple in their mouth. See Causes of Sore Nipples, and Why Does Breastfeeding Hurt? and check in with your breastfeeding specialist as soon as possible.
Baby not getting enough milk
There are several ways to tell if your baby is getting enough milk and sometimes more may be needed than a mother can pump. Or there may be plenty of milk but once your baby starts to latch on they may not be very efficient at breastfeeding at first and may still need supplementary feeds for a while to ensure they are getting enough milk. The following links have more information:
- How to Make More Breast Milk
- Baby Not Gaining Weight
- Supplementing an Underweight Baby
- Breastfeeding a Sleepy Baby
Summary
There are various reasons why a baby can’t breastfeed when they are first born. Until your baby can get the hang of breastfeeding it’s important to (1) express your breast milk and (2) keep your baby well fed. Expressing breast milk frequently will protect and stimulate your milk supply and provide a milk supplement for your baby. Keeping your baby well fed ensures they are contented and have the energy to learn to breastfeed. Keeping your baby close to you in skin-to-skin contact where possible will help promote your baby’s instinctive feeding behaviours. Most of the challenges that prevent a baby breastfeeding can be overcome with time, patience and skilled help. The support of a breastfeeding specialist can be invaluable.


